Understanding Arm Pain, Numbness & “Heaviness” – And What You Can Do About It
At Rx Physiotherapy, we often see people who describe:
-
Arm pain that doesn’t quite follow a nerve pattern
-
Tingling into the hand (often the little finger side)
-
A feeling of heaviness when the arm is overhead
-
Weakness or fatigue during everyday tasks
-
Swelling or colour changes in rare cases
One possible cause of these symptoms is Thoracic Outlet Syndrome (TOS).
Let’s break it down clearly.
What is Thoracic Outlet Syndrome?
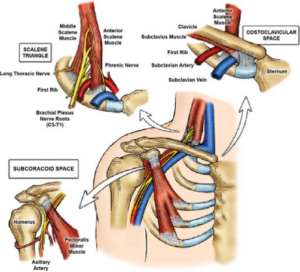
Thoracic Outlet Syndrome occurs when nerves or blood vessels are compressed as they travel from your neck into your arm.
The compression happens in a region called the thoracic outlet — the space between:
-
The collarbone
-
The first rib
-
Surrounding muscles (like the scalenes and pectoralis minor)
Three structures pass through this area:
-
The brachial plexus (nerves to the arm)
-
The subclavian artery
-
The subclavian vein
Depending on which structure is irritated, symptoms can vary.
The three types of TOS
 Neurogenic TOS (Most Common)
Neurogenic TOS (Most Common)
This involves irritation of the nerves.
You may experience:
-
Tingling or numbness
-
Diffuse arm pain
-
Weakness in the hand
-
A heavy or fatigued feeling, especially overhead
 Venous TOS (Less Common)
Venous TOS (Less Common)
This affects the vein.
Symptoms may include:
-
Swelling
-
Bluish colour changes
-
Tightness in the arm
 Arterial TOS (Rare)
Arterial TOS (Rare)
This affects the artery and may cause:
-
Cold sensitivity
-
Pale skin
-
Cramping or fatigue with activity
If vascular symptoms are suspected, urgent medical assessment is required.
Guidelines from the Society for Vascular Surgery help clinicians differentiate these types appropriately.
Why does it happen?
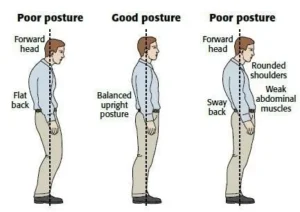
TOS is usually not caused by “something being out of place.”
Instead, it’s typically a load and space problem.
Contributing factors can include:
-
Forward head posture
-
Rounded shoulders
-
Poor scapular control
-
Tight anterior shoulder muscles
-
Repetitive overhead work
-
Heavy carrying
-
Previous trauma
Research in shoulder biomechanics (including work by Ludewig) shows that scapular positioning and movement influence how much space exists in this region.
In many cases, symptoms are position-dependent and load-dependent, which is good news — because that means they’re modifiable.
How is TOS diagnosed?
There is no single scan or test that “proves” neurogenic TOS.
Diagnosis is primarily clinical and based on:
-
Your symptom pattern
-
Reproduction of familiar symptoms with specific arm positions
-
Ruling out other causes such as cervical radiculopathy or peripheral nerve entrapment
Research reviews (such as those by Povlsen) confirm that diagnosis is based on a cluster of findings rather than one definitive test.
At Rx Physiotherapy, we perform:
-
Cervical spine assessment
-
Scapular movement analysis
-
Neural provocation testing
-
Strength and endurance testing
-
Vascular screening when indicated
Our priority is always to rule out serious causes first.
Can Physiotherapy help?
Yes — especially in neurogenic TOS.
Systematic reviews (e.g., Peek et al.) show that structured conservative rehabilitation can significantly improve symptoms in many patients.
Improvement rates reported in studies range between 50–90% in appropriate cases.
What does treatment involve?
At Rx Physiotherapy, treatment is structured and progressive.
 Phase 1 – Calm the Irritation
Phase 1 – Calm the Irritation
-
Reduce aggravating positions
-
Modify overhead loading
-
Improve scapular positioning
-
Gentle mobility work
 Phase 2 – Restore Control
Phase 2 – Restore Control
-
Serratus anterior activation
-
Lower trapezius strengthening
-
Postural endurance training
-
Gradual reintroduction of overhead movement
 Phase 3 – Build Capacity
Phase 3 – Build Capacity
-
Strength training
-
Overhead load tolerance
-
Work or sport-specific integration
TOS is rarely fixed with passive treatment alone.
Exercise-based rehabilitation is key.
When is surgery needed? 
Surgery is typically reserved for:
-
Confirmed vascular TOS
-
Structural compression (e.g., cervical rib)
-
Cases that fail structured conservative management
Guidelines from the Society for Vascular Surgery outline when surgical referral is appropriate.
Most neurogenic TOS cases improve with conservative management.
When should you seek assessment?
Book an assessment if you notice:
-
Persistent arm tingling or heaviness
-
Symptoms that worsen overhead
-
Swelling or colour changes in the arm
-
Unexplained weakness in the hand
Early assessment improves outcomes.
The good news 
Thoracic Outlet Syndrome can sound intimidating.
But in most cases, it is:
-
Load-related
-
Mechanically influenced
-
Responsive to targeted rehabilitation
With the right approach, symptoms can significantly improve.”