Plantar Fasciitis Treatment
PLANTAR FASCIITIS TREATMENT AT RX PHYSIOTHERAPY
At Rx Physiotherapy, we understand how frustrating heel pain can be — especially when it limits your ability to walk, run, or even get through the day comfortably.
Plantar fasciitis isn’t just a “foot problem.”
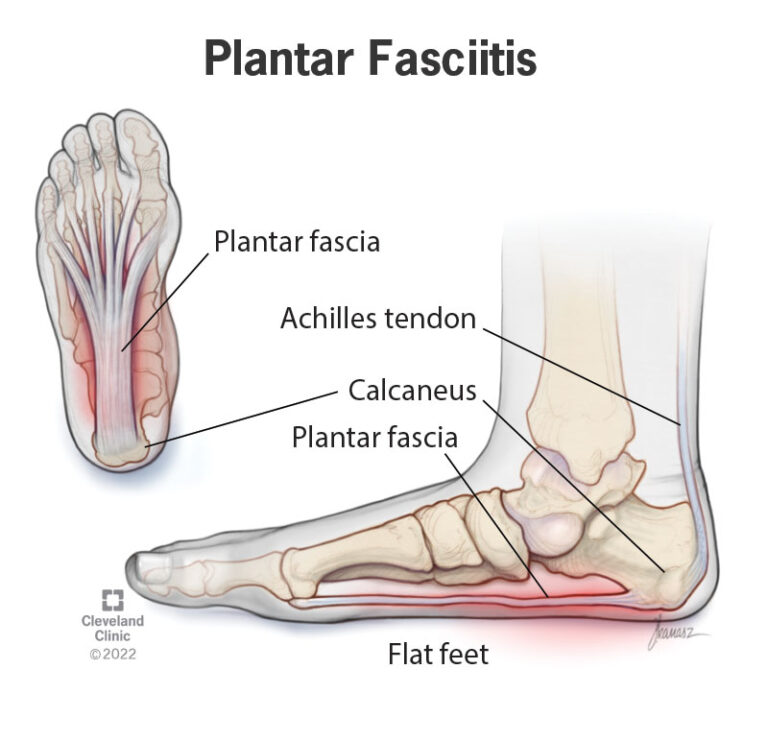
It’s a load-related condition involving irritation of the plantar fascia — a thick band of tissue that supports your arch and helps transfer force when you move.
Our approach is simple:
Reduce your pain, restore your movement, and build your capacity so your feet can handle load again.

What is plantar fasciitis?
Plantar fasciitis (more accurately described as plantar fasciopathy) is a condition involving irritation and degeneration of the plantar fascia, rather than purely inflammation.
It typically presents as:
- Pain under the heel (especially first steps in the morning)
- Pain after periods of rest
- Symptoms that ease with movement but worsen with prolonged load
- Tenderness at the base of the heel
This condition is very common, particularly in active individuals and those with increased load demands.
Why does it happen?
Plantar fasciitis develops when the load placed on the foot exceeds its capacity to tolerate it.
Common contributing factors include:
- Sudden increases in activity (running, walking, sport)
- Reduced calf strength or endurance
- Limited ankle mobility (especially dorsiflexion)
- Prolonged standing or walking
- Foot strength and control deficits
- Changes in footwear
Importantly:
It’s not just inflammation — it’s a capacity problem.
Who We Treat
- Runners with heel pain during or after training
- Gym members struggling with loaded lower body work
- Occupations involving prolonged standing (healthcare, retail, trades)
- People returning to exercise after a break
- Anyone with persistent “first step” heel pain
From everyday activity to high performance — we guide you back.
Movement is Medicine
Best-practice management of plantar fasciitis focuses on progressive loading, not rest alone.
Research supports:
✔ Strength-based rehab for long-term improvement
✔ Gradual loading of the plantar fascia and calf complex
✔ Avoiding complete unloading where possible
While short-term symptom relief strategies can help,
lasting improvement comes from restoring load tolerance.
Our Approach to Plantar Fasciitis Rehabilitation
At Rx Physiotherapy, we take a structured, individualised approach — no generic programs, no guesswork.
We start by understanding you and your loading patterns.
- Thorough assessment of foot, ankle, and lower limb
- Identify contributing factors (mobility, strength, training loads)
- Screen for alternative diagnoses (e.g. nerve-related pain, stress injury)
- Clear explanation of your condition
- Structured rehab plan
You leave your first session knowing exactly what’s going on and what to do next.
Early management focuses on reducing irritation while staying active.
- Modify aggravating loads (not complete rest)
- Footwear and activity guidance
- Short-term pain relief strategies (e.g. taping, isometrics)
- Gentle mobility and calf loading
Complete rest is not recommended, as it may delay recovery.
Now we rebuild your foundation.
- Progressive calf strengthening (key driver of outcomes)
- Introduce plantar fascia-specific loading
- Improve ankle mobility
- Develop foot strength and control
Heavy-slow resistance training has been shown to be effective in improving pain and function over time.
Once your symptoms are controlled, we progress toward full function.
- Load tolerance for walking, running, and sport
- Plyometric and dynamic loading (when appropriate)
- Return-to-running or training programs
- Build resilience in the entire lower limb
Plantar fasciitis can return if underlying capacity isn’t addressed.
We focus on:
- Long-term strength and load management
- Foot and calf conditioning
- Training structure and progression
- Footwear guidance where needed

It’s Not Just Your Foot
Plantar fasciitis is influenced by the entire lower limb and how you move.
We consider:
- Calf strength and endurance
- Achilles tendon loading
- Hip and lower limb control
- Training loads and recovery
This is why isolated treatments don’t work long term — the whole system needs to adapt.
Education and Empowerment
Understanding your condition is key to recovery.
We help you:
- Understand what’s driving your pain
- Know what activities are safe (and helpful)
- Manage symptoms without fear
- Progress confidently back to full activity

YOUR PARTNER IN RECOVERY
At Rx Physiotherapy, we combine:
- Evidence-based treatment
- Individualised rehab
- Strength-focused recovery
- Ongoing support
Because the goal isn’t just to settle your heel pain —
it’s to build a foot that can handle whatever you throw at it.
Want to Learn More?
Plantar fasciitis is one of the most common causes of heel pain — but also one of the most misunderstood.
Most cases improve with: Education, Load management &Progressive strengthening
The goal isn’t just pain relief — it’s long-term resilience.





